Ectopic Pregnancy Following Interval Tubal Sterilization
Lessons Learnt
DOI:
https://doi.org/10.22502/jlmc.v5i2.139Keywords:
contraception, ectopic, pregnancy, salpingectomy, tubal sterilizationAbstract
Introduction: Tubal sterilization is a highly effective method of permanent contraception. However, pregnancy can still occur following a successful procedure. Published literatures report a failure rate of 0.13-1.3% and 15-33% of such pregnancies are likely to be ectopic.
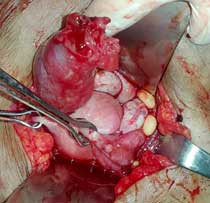
Case report: A 33 years para three lady with prior history of tubal ligation presented with generalized abdominal pain and several episodes of vomiting. Bimanual examination revealed a soft and mobile mass of 2 x 3 cm in right adnexa. Urine pregnancy test was positive and ultrasonogram showed a heterogeneous mass of 3.4 x 3.3 cm in right adnexa with empty uterine cavity. Culdocentesis resulted in aspiration of frank non-clotting blood. She then underwent emergency laparotomy with bilateral salpingectomy for ruptured ectopic pregnancy.
Conclusion: Ectopic pregnancy after tubal sterilization though rare is not entirely impossible. All women who are offered this procedure should always be educated about its failure rate. And in women presenting with acute abdomen, a prior history of tubal sterilization doesn't preclude the possibility of ectopic pregnancy.
Downloads
Published
Issue
Section
License
- The Journal of Lumbini Medical College (JLMC) publishes open access articles under the terms of the Creative Commons Attribution (CC BY) License which permits use, distribution and reproduction in any medium, provided the original work is properly cited.
- JLMC requires an exclusive licence to publish the article first in its journal in print and online.
- The corresponding author should read and agree to the following statement before submission of the manuscript for publication,
- License agreement
- In submitting an article to Journal of Lumbini Medical College (JLMC) I certify that:
- I am authorized by my co-authors to enter into these arrangements.
- I warrant, on behalf of myself and my co-authors, that:
- the article is original, has not been formally published in any other peer-reviewed journal, is not under consideration by any other journal and does not infringe any existing copyright or any other third party rights;
- I am/we are the sole author(s) of the article and have full authority to enter into this agreement and in granting rights to JLMC are not in breach of any other obligation;
- the article contains nothing that is unlawful, libellous, or which would, if published, constitute a breach of contract or of confidence or of commitment given to secrecy;
- I/we have taken due care to ensure the integrity of the article. To my/our - and currently accepted scientific - knowledge all statements contained in it purporting to be facts are true and any formula or instruction contained in the article will not, if followed accurately, cause any injury, illness or damage to the user.
- I, and all co-authors, agree that the article, if editorially accepted for publication, shall be licensed under the Creative Commons Attribution License 4.0. If the law requires that the article be published in the public domain, I/we will notify JLMC at the time of submission, and in such cases the article shall be released under the Creative Commons 1.0 Public Domain Dedication waiver. For the avoidance of doubt it is stated that sections 1 and 2 of this license agreement shall apply and prevail regardless of whether the article is published under Creative Commons Attribution License 4.0 or the Creative Commons 1.0 Public Domain Dedication waiver.
- I, and all co-authors, agree that, if the article is editorially accepted for publication in JLMC, data included in the article shall be made available under the Creative Commons 1.0 Public Domain Dedication waiver, unless otherwise stated. For the avoidance of doubt it is stated that sections 1, 2, and 3 of this license agreement shall apply and prevail.
Please visit Creative Commons web page for details of the terms.










