Trend of Breastfeeding and its Impact on Morbidity in Children in a Tertiary Care Hospital in Kathmandu
DOI:
https://doi.org/10.22502/jlmc.v7i1.262Keywords:
breastfeeding, acute respiratory infections, acute otitis media, acute diarrheal episodesAbstract
Introduction: WHO advocates for exclusive breastfeeding in infants till six months of age. Exclusive breastfeeding has been estimated to reduce 70% of infection related mortality in children. This study aims to elaborate the current trend of breastfeeding and its impact on common infectious morbidities in children.
Methods: This study was a prospective longitudinal study done at Kathmandu Medical College Teaching Hospital with a sample size of 103 infants. Detailed proforma including sociodemographic data, breastfeeding related data and morbidities were collected at one and half months of life. The patients were followed up at 6 months of age again and the same proforma was again filled up. Statistical analysis was done with SPSS 20.0 and various associations were elucidated.
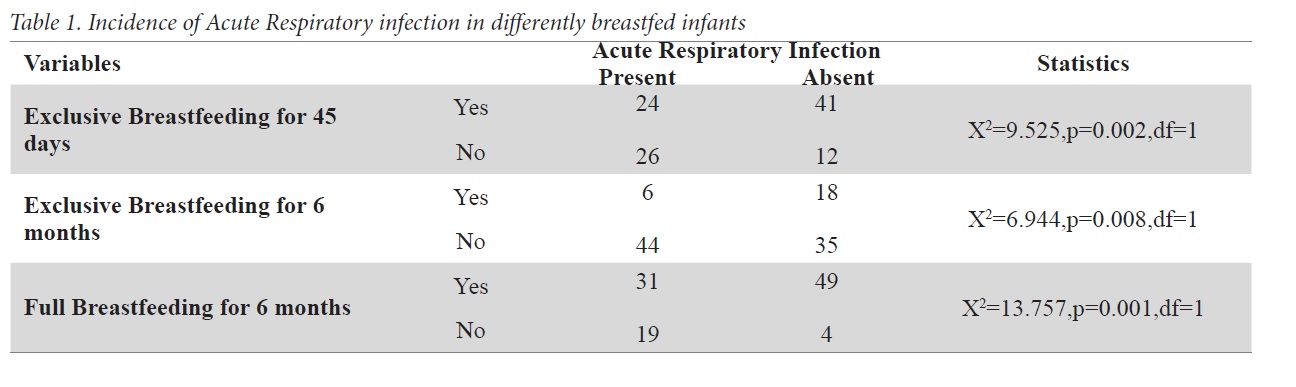
Results: A total of 103 infants were analyzed. Males were 58 in numbers with mean birth weight of the infants being 3048±537 grams. Breast feeding was initiated within an hour in around 37%. At one and half months of age, 63% reported of exclusive breastfeeding which decreased to 23% at 6 months of age. Breastfeeding for at least 45 days decreased the incidence of Acute Respiratory Infections(ARI), Acute Otitis Media(AOM) and diarrheal diseases although statistically significant difference was found with only ARIs.
Conclusion: Prevalence of exclusive breastfeeding is low in the study. The study has also shown that breastfeeding significantly reduces incidence of common infectious morbidities in infants.
Downloads
References
American Academy of Pediatrics. Breastfeeding and the Use of Human Milk. Vol. 129, PEDIATRICS. 2012 Mar. DOI: 10.1542/peds.2011-3552
UNICEF. Infant and Young Child Feeding Global Database. 2016. https://data.unicef.org/topic/nutrition/infant-and-young-child-feeding/
Horta B., Victora C. Short-term effects of breastfeeding: a systematic review on the benefits of breastfeeding on diarrhoea and pneumonia mortality. World Health Organization. 2013. http://www.who.int/iris/handle/10665/95585
WHO. WHO Fact sheet, Children: reducing mortality. 2016. http://www.who.int/mediacentre/factsheets/fs178/en/
Jones G, Steketee RW, Black RE, Bhutta ZA, Morris SS, Bellagio Child Survival Study Group. How many child deaths can we prevent this year? Lancet. 2003 Jul 5;362(9377):65–71.DOI: 10.1016/S0140-6736(03)13811-1
Victora CG, Bahl R, Barros AJD, França GVA, Horton S, Krasevec J, et al. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet. 2016 Jan;387(10017):475–90. DOI:10.1016/S0140-6736(15)01024-7
Patil CL, Turab A, Ambikapathi R, Nesamvuni C, Chandyo RK, Bose A, et al. Early interruption of exclusive breastfeeding: results from the eight-country MAL-ED study. J Heal Popul Nutr. 2015 Dec 1;34(1):10. PMID: 26825923
WHO. Indicators for assessing breastfeeding practices WHO/CDD/SER/91.14. World Health Organization. 1991. p. 1–14. http://apps.who.int/iris/bitstream/10665/62134/1/WHO_CDD_SER_91.14.pdf
Betrán AP, Ye J, Moller A-B, Zhang J, Gülmezoglu AM, Torloni MR. The Increasing Trend in Caesarean Section Rates: Global, Regional and National Estimates: 1990-2014. PLoS One. 2016;11(2):e0148343. PMID: 26849801
Dns G, Prasuti Tatha Prajanan Swasthya Kendra A. Rising Cesarean Section Rates in Nepal: Question of safety and Integrity on Obstetric Emergency Practice. 2017;7. DOI: 10.19080/JGWH.2017.07.555716
Chhetri S, Singh U. Caesarean section: its rates and indications at a tertiary referral center in Eastern Nepal. Heal Renaiss. 2011;9(3):179–83. DOI: 10.3126/hren.v9i3.5587
ICF M of H and PNE. Nepal Demographic and Health Survey 2016 Key Indicators Report Ministry of Health Ramshah Path, Kathmandu Nepal New ERA Ministry of Health. 2017 . Available from: www.DHSprogram.com.
World Bank Gender Data Portal | Country - Nepal. Available from: http://datatopics.worldbank.org/gender/country/nepal
Department of Health Services. Annual Report 2014/15. Kathmandu;
Ip S, Chung M, Raman G, Chew P, Magula N, DeVine D, et al. Breastfeeding and maternal and infant health outcomes in developed countries. Evid Rep Technol Assess. 2007 Apr;(153):1–186. PMID: 17764214
Nishimura T, Suzue J, Kaji H. Breastfeeding reduces the severity of respiratory syncytial virus infection among young infants: A multi-center prospective study. Pediatr Int.2009;51(6):812–6. PMID: 19419530
Abdullah A, Hort K, Butu Y, Simpson L. Risk factors associated with neonatal deaths: a matched case–control study in Indonesia. Glob Health Action. 2016 Dec 16;9(1):30445. PMID: 28157054
Sankar MJ, Sinha B, Chowdhury R, Bhandari N, Taneja S, Martines J, et al. Optimal breastfeeding practices and infant and child mortality: a systematic review and meta-analysis. Acta Paediatr. 2015 Dec;104(S467):3–13. DOI: 10.1111/apa.13147
Bowatte G, Tham R, Allen K, Tan D, Lau M, Dai X, et al. Breastfeeding and childhood acute otitis media: a systematic review and meta-analysis. Acta Paediatr. 2015 Dec;104:85–95.DOI: 10.1111/apa.13151
Boone KM, Geraghty SR, Keim SA. Feeding at the Breast and Expressed Milk Feeding: Associations with Otitis Media and Diarrhea in Infants. J Pediatr. 2016 Jul;174:118–25. PMID: 27174145
Lamberti LM, Fischer Walker CL, Noiman A, Victora C, Black RE. Breastfeeding and the risk for diarrhea morbidity and mortality. BMC Public Health. 2011 Apr 13;11(Suppl 3):S15. PMID: 21501432
Downloads
Published
Issue
Section
License
- The Journal of Lumbini Medical College (JLMC) publishes open access articles under the terms of the Creative Commons Attribution (CC BY) License which permits use, distribution and reproduction in any medium, provided the original work is properly cited.
- JLMC requires an exclusive licence to publish the article first in its journal in print and online.
- The corresponding author should read and agree to the following statement before submission of the manuscript for publication,
- License agreement
- In submitting an article to Journal of Lumbini Medical College (JLMC) I certify that:
- I am authorized by my co-authors to enter into these arrangements.
- I warrant, on behalf of myself and my co-authors, that:
- the article is original, has not been formally published in any other peer-reviewed journal, is not under consideration by any other journal and does not infringe any existing copyright or any other third party rights;
- I am/we are the sole author(s) of the article and have full authority to enter into this agreement and in granting rights to JLMC are not in breach of any other obligation;
- the article contains nothing that is unlawful, libellous, or which would, if published, constitute a breach of contract or of confidence or of commitment given to secrecy;
- I/we have taken due care to ensure the integrity of the article. To my/our - and currently accepted scientific - knowledge all statements contained in it purporting to be facts are true and any formula or instruction contained in the article will not, if followed accurately, cause any injury, illness or damage to the user.
- I, and all co-authors, agree that the article, if editorially accepted for publication, shall be licensed under the Creative Commons Attribution License 4.0. If the law requires that the article be published in the public domain, I/we will notify JLMC at the time of submission, and in such cases the article shall be released under the Creative Commons 1.0 Public Domain Dedication waiver. For the avoidance of doubt it is stated that sections 1 and 2 of this license agreement shall apply and prevail regardless of whether the article is published under Creative Commons Attribution License 4.0 or the Creative Commons 1.0 Public Domain Dedication waiver.
- I, and all co-authors, agree that, if the article is editorially accepted for publication in JLMC, data included in the article shall be made available under the Creative Commons 1.0 Public Domain Dedication waiver, unless otherwise stated. For the avoidance of doubt it is stated that sections 1, 2, and 3 of this license agreement shall apply and prevail.
Please visit Creative Commons web page for details of the terms.










